Metronidazole Cumulative Dose Calculator
Use this tool to track your total Metronidazole intake. Research indicates that the risk of neuropathy increases significantly after a cumulative dose of 42 grams.
Detailed risk assessment based on cumulative intake.
Imagine waking up one morning and feeling like you're walking on cotton balls, or perhaps experiencing a sudden, sharp electric shock in your fingertips for no apparent reason. For most, these sensations are frightening and confusing. However, if you've been taking a specific antibiotic for a few weeks or months, these aren't just random glitches in your nervous system. You might be experiencing Metronidazole neuropathy is a neurological complication where the antibiotic damages peripheral nerves, leading to sensory loss and pain.
While this medication is a lifesaver for treating stubborn infections, it has a hidden threshold. Once you cross a certain cumulative dose, your risk of nerve damage doesn't just increase-it spikes. The good news is that if you catch it early, the damage is often reversible. The bad news? If you ignore the tingling, you could be looking at permanent disability.
Quick Takeaways on Metronidazole Nerve Damage
- The Danger Zone: Risk increases significantly after a cumulative dose of 42 grams.
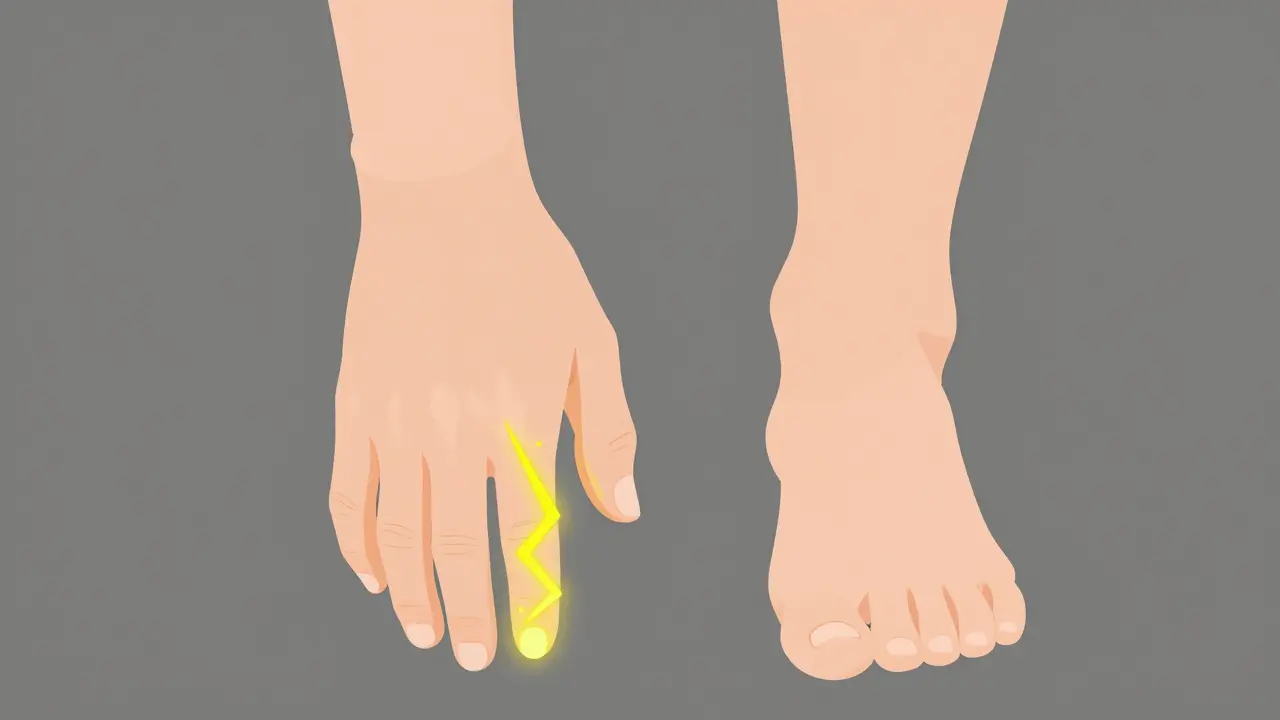
- Primary Symptoms: Numbness, tingling (paresthesia), and burning pain, usually starting in the feet.
- The Recovery Key: Immediate discontinuation of the drug is the only way to stop the progression.
- Success Rate: About 94% of patients see improvement or full recovery if the drug is stopped promptly.
What Exactly is Metronidazole Neuropathy?
To understand this condition, we first need to look at the drug itself. Metronidazole is a nitroimidazole antibiotic used to treat anaerobic bacteria and protozoal infections. You might know it by the brand name Flagyl. It's incredibly effective for things like bacterial vaginosis, giardiasis, or severe abdominal infections. However, because it can cross the blood-brain barrier, it doesn't just target bacteria; it can interfere with your neurons.
This specific type of damage is called peripheral neuropathy, which means the nerves outside your brain and spinal cord are malfunctioning. In the case of metronidazole, the drug's nitro group can create reactive intermediates in your nerve tissues. This leads to neuronal swelling and degeneration. Essentially, the "wires" sending signals from your toes and fingers to your brain start to fray, leaving you with distorted sensations or a complete lack of feeling.
Recognizing the Warning Signs
Neuropathy doesn't usually hit you all at once. It's a slow creep. Most people describe a "stocking-glove" distribution, meaning the numbness starts at the furthest points-your toes and fingertips-and slowly moves up your legs and arms.
Keep an eye out for these specific sensations:
- Paresthesia: That "pins and needles" feeling you get when your foot falls asleep, but it doesn't go away.
- Burning Sensations: A feeling of intense heat or "fire" in the soles of the feet, which often gets worse at night.
- Electric Shocks: Sudden, stabbing pains that feel like a low-voltage current running through your limbs.
- Temperature Issues: Some patients report an odd inability to regulate temperature in their extremities, sometimes feeling a need to soak their feet in ice water to dull the pain.
It's easy to dismiss these as "just getting older" or "bad circulation," but if you're on a course of antibiotics, these are red flags that require immediate medical attention.
The 42-Gram Threshold: Why Dose Matters
Not everyone who takes metronidazole will develop neuropathy. In fact, for short-term use, it's generally very safe. The real risk emerges with prolonged therapy or high doses. Research has identified a critical tipping point at 42 grams of cumulative exposure. To put that in perspective, if you're taking the standard 500mg dose three times a day, you'll hit that 42-gram mark in about four weeks.
| Total Dose Received | Neuropathy Incidence Rate | Risk Level |
|---|---|---|
| ≤ 42 Grams | 1.7% | Low |
| > 42 Grams | 17.9% | High (10.5x Increase) |
While most people don't see symptoms until 4 to 6 months of treatment, high-dose regimens can trigger these effects in as little as 10 days. This dose-dependency is why clinicians are now being urged to monitor patients more closely as they approach the one-month mark of treatment.
Is it Metronidazole or Something Else?
One of the biggest dangers with this condition is misdiagnosis. Because the symptoms-numbness and tingling-are so common, doctors often look for more "likely" culprits first. This is especially true for patients who already have diabetes, as clinicians may assume it's simply diabetic neuropathy.
However, there are key differences. Metronidazole neuropathy often appears suddenly in relation to drug use and can involve autonomic features (like the temperature dysregulation mentioned earlier). Unlike some chemotherapy drugs that cause permanent nerve death, metronidazole toxicity is often reversible if caught in time. It's also different from metronidazole-induced encephalopathy, which affects the brain and causes confusion or loss of coordination, rather than just tingling in the limbs.
What to Do If You Suspect Nerve Damage
If you are currently taking this medication and notice any change in sensation, the most important step is to contact your doctor immediately. Do not wait for your next scheduled appointment. The window for a full recovery closes quickly once the nerves begin to degenerate.
Here is what the clinical process usually looks like:
- Immediate Cessation: Your doctor will likely stop the metronidazole immediately. This is the only way to prevent further axonal damage.
- Diagnostic Testing: You might undergo an Electromyography (EMG) or nerve conduction study. This test measures the electrical activity in your muscles and nerves to confirm if the damage is axonal or demyelinating.
- Alternative Therapy: If you still have an active infection, your doctor will switch you to a different antibiotic that doesn't carry the same neurotoxic risk.
- Rehabilitation: In some cases, structured physical therapy is recommended. Evidence shows that aggressive rehab can help patients regain a normal gait significantly faster than those who just wait for the nerves to heal on their own.
Long-Term Outlook and Recovery
For the vast majority of people, the prognosis is positive. Around 94% of cases show at least partial recovery. Some people feel the tingling vanish within two weeks of stopping the drug. For others, the road is longer; there are documented cases where it took six months of rehabilitation before nerve function returned to normal.
Unfortunately, about 6% of patients may suffer permanent disability. This is why the "42-gram rule" is so vital. When the drug is stopped early, the neurons have a chance to repair themselves. When the drug is continued despite symptoms, the damage can become irreversible.
How long does it take for the numbness to go away after stopping the drug?
Recovery times vary. Some patients notice a significant improvement within 14 days, while others may take several months. In a few cases, complete resolution of symptoms took up to 6 months of recovery and physical therapy.
Can I take vitamins like B12 to fix the tingling?
While B-vitamins are essential for nerve health, they cannot "neutralize" the toxic effects of metronidazole. The primary treatment is the immediate cessation of the drug. Some research is currently looking into alpha-lipoic acid as a potential neuroprotective agent, but this should only be done under medical supervision.
Is a metallic taste in my mouth a sign of neuropathy?
No. A metallic taste and dry mouth are very common, mild side effects of metronidazole. While annoying, they are not indicators of nerve damage. Neuropathy is characterized by sensory changes like numbness, tingling, or pain in the extremities.
Will this happen if I only take the medicine for a week?
It is very unlikely. The risk is primarily associated with prolonged use or extremely high doses. Most patients who develop neuropathy have exceeded a cumulative dose of 42 grams, which typically happens after several weeks of treatment.
Should I be worried if I have diabetes and feel tingling while on this drug?
Yes. Because diabetic neuropathy and drug-induced neuropathy look similar, there is a high risk of misdiagnosis. If you are on metronidazole and notice a change or worsening of tingling, inform your doctor immediately so they can determine if the drug is exacerbating your condition.
Next Steps for Patients and Caregivers
If you or a loved one are currently on a long-term course of metronidazole, don't panic, but do stay vigilant. A simple way to monitor is to do a "sensory check" once a week-check if you can feel the texture of your socks or if there's any new tingling in your fingers.
If you've already stopped the medication and are still feeling symptoms, focus on physical activity. Gentle movement and physical therapy can help maintain muscle function while the nerves slowly regenerate. If the pain is severe, talk to your doctor about neuropathic pain medications, though remember that these treat the symptoms, not the cause.



Sam Hayes
April 5, 2026 AT 08:41glad this got posted because a lot of people just ignore the tingling until it is too late and the 42 gram mark is a really useful metric for anyone tracking their meds
Joseph Rutakangwa
April 7, 2026 AT 05:38good info here keep an eye on your toes
Rob Newton
April 7, 2026 AT 15:51Too much hand-holding. Just read the pamphlet.
Joey Petelle
April 8, 2026 AT 07:15Oh look at us, terrified of a few sparks in our fingertips while the glorious American pharmaceutical complex just bills us for the privilege of feeling like we're wearing invisible wool socks. It's almost poetic how we trust a pill to save us and then act shocked when our nerves decide to go on strike like a union meeting in the middle of July. Truly an enlightened age we live in where we measure our health in grams of toxicity before we realize the 'wires are fraying' and we're basically becoming human static. Absolutely precious.
Lawrence Rimmer
April 8, 2026 AT 09:29The irony of pharmacological intervention is that we trade one misery for another, yet we call it progress. This text simplifies a complex neural degradation into a mere checklist, ignoring the existential dread of losing somatic sensation.
Will Baker
April 9, 2026 AT 23:08I'm sure the '42 gram rule' is just a lucky guess by some researcher who wanted to get published. Maybe the nerves just get bored of the drug and decide to quit. Who knows?
Mark Zhang
April 11, 2026 AT 18:19I really appreciate the reminder about the diabetic overlap. It can be so scary when you aren't sure if it's your chronic condition or a new reaction, so knowing there's a path to recovery is a huge relief.
Aysha Hind
April 11, 2026 AT 21:00Total shill post. They want you to trust the 'recovery rate' so you keep using their poison. Ever notice how they just tell you to switch to another antibiotic? It's a revolving door of chemicals designed to keep us numb and compliant while the real cause of these 'glitches' is probably something they aren't mentioning in the footnotes of this sanitized little guide. Wake up and stop blindly trusting the white coats who treat us like lab rats in a maze.
angel sharma
April 12, 2026 AT 12:41This is exactly the kind of awareness we need to spread because if we all stay vigilant and support each other in monitoring these side effects we can actually push for better patient safety and ensure that nobody has to suffer through permanent nerve damage just because they didn't know about a cumulative dose threshold that should be common knowledge for every single person prescribed this medication in the first place!
Dipankar Das
April 13, 2026 AT 21:35It is absolutely imperative that patients adhere to the medical guidance provided here without hesitation. Any individual who chooses to ignore these symptoms is displaying a reckless disregard for their own well-being and must be corrected immediately. You must act now to secure your health!
Vicki Marinker
April 15, 2026 AT 01:45The prose is dreadfully simplistic and the formatting is amateurish at best.
Beth LeCours
April 16, 2026 AT 10:45too long didnt read
Dee McDonald
April 16, 2026 AT 20:57Wait, so if I'm already feeling the burning sensation, does that mean I've already hit the 42 gram mark or could it happen sooner for some people? I want to make sure we're all understanding that individual biology varies and we can't just rely on one number for everyone!
Ace Kalagui
April 18, 2026 AT 12:52I've seen so many people in different communities struggle with antibiotic side effects and it's always such a journey of trial and error, so I really want to encourage everyone to keep a detailed log of their dosages and how they feel every single day because that data is what actually helps the doctors make the right call and gets us back on our feet faster than just waiting around for things to magically fix themselves.
Hope Azzaratta-Rubyhawk
April 19, 2026 AT 02:43YOU MUST NOT NEGLECT THIS. If you feel a single tingle in your toe, you must call your physician this instant. There is no room for complacency when permanent disability is on the line!